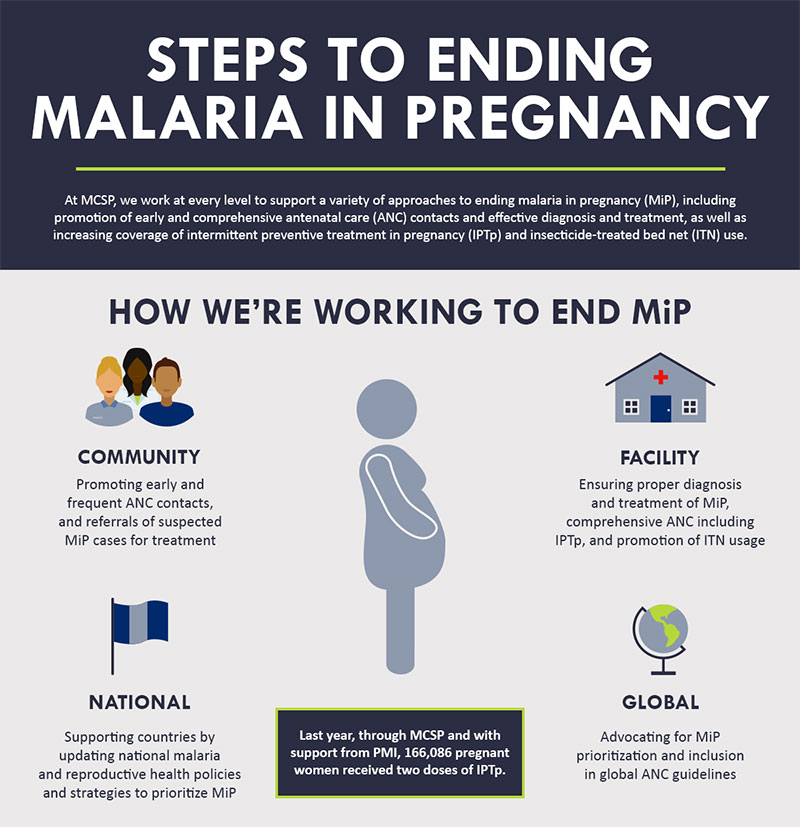
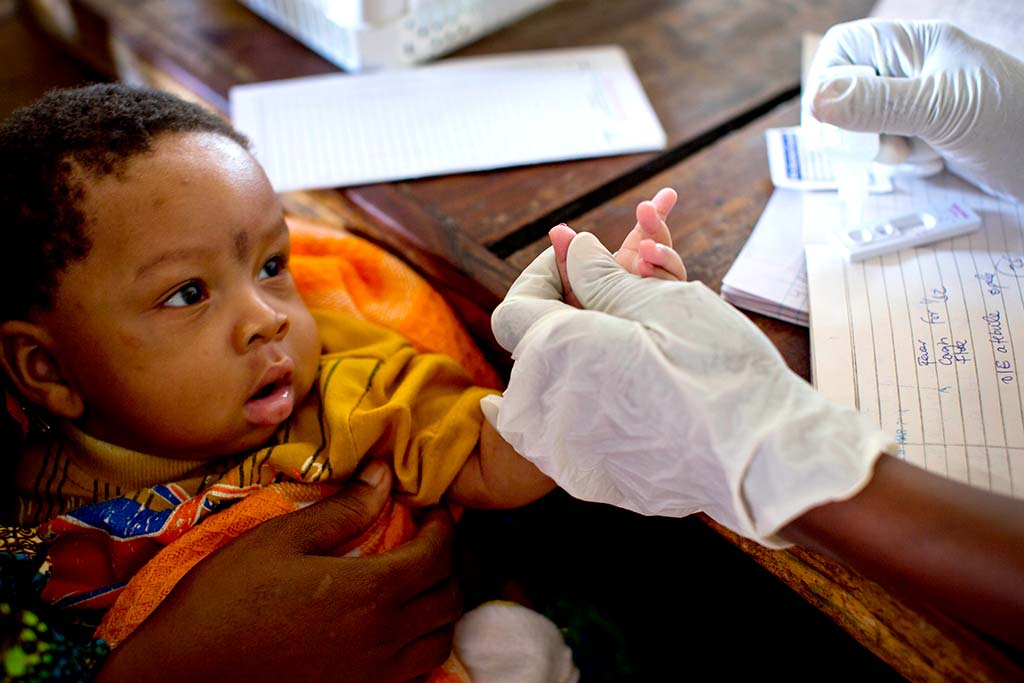
Malaria
One Disease, Many Faces
By Katrin DeCamp and Joel Bobeck
Children in Burkina Faso, where MCSP is supporting malaria in pregnancy operational research. (All video courtesy of Jhpiego)
There are many compelling reasons to eliminate malaria now.
As the effects of climate change threaten to reverse the gains made in combatting the disease, mosquitoes are becoming more resistant to the drugs and insecticides traditionally used to fight them. “Malaria superbugs” – scientists warn us – may be putting us on the losing side of this battle. It took four years to eliminate malaria in the United States, but our seven-decade fight to do so globally continues.
However, there is much to be hopeful about.
Scale-up of malaria prevention and treatment efforts – including widespread use of treated bed nets – led to a 60% global decline in malaria deaths between 2000 and 2015. Ten countries that had the disease in 2000 are now malaria free. And in sub-Saharan Africa, the region hardest hit by the disease, access to malaria tools and services is dramatically increasing for those most vulnerable – pregnant women and children. Moreover, cutting edge treatments in development may keep us ahead of the deadly impact of the disease.

But what will it take to close the gaps that remain?
MCSP-trained community health workers in Kenya visit families to share messages on prevention of malaria in pregnancy, and the importance of early and regular antenatal care contacts, use of mosquito nets, and following malaria treatment protocols.

MCSP is playing a key role in ending malaria for good.
Our work throughout Africa — and Burma in South East Asia — aims to ensure that all people at risk for the disease have access to preventative, diagnostic and treatment services. Our focus remains on the most vulnerable (pregnant women and young children) while helping to strengthen health systems comprehensively to ensure increased coverage and lasting results. This includes malaria in pregnancy prevention and control, improving the case management of childhood diseases at both the health facility and community level, and extending our reach through community level grants.
We’re all about coverage.
What stands between more needless deaths and elimination of a disease that threatens nearly half of the world’s population? Reaching the “unreachable” by testing new innovations – such as community distribution of IPTp-SP (intermittent preventive treatment in pregnancy with sulfadoxine-pyrimethamine) – and ensuring all women are educated on malaria in pregnancy. At both community and facility levels, we must also promptly diagnose and effectively treat every child with fever.
Investment in effective approaches is essential to defeating the disease.
Midwifery students in Burma learn the risks malaria poses to pregnant women and children. MCSP is working with the Ministry of Health and Sports to provide national technical assistance to strengthen antenatal care services and case management for pregnant women and children.
We’re building on our successes and learning from our challenges to propel our malaria programs to the next level.
In collaboration with the Roll Back Malaria (RBM) partnership and the President’s Malaria Initiative (PMI), we’re working tirelessly to improve coverage of high-impact interventions and achieve results at scale. At the global level, MCSP provides strategic leadership and collaborates closely with RBM Initiative partners and the World Health Organization (WHO) to accelerate progress. We’re adapting our efforts to local requirements to achieve a 100% increase in IPTp-SP coverage from current levels by 2020, and national coverage of at least 90% by 2030.
MCSP supports the PMI/USAID goal of reducing malaria deaths by half in target countries by reaching at least 85% of the most vulnerable groups (children under five and pregnant women) with proven and effective prevention and treatment measures. PMI/USAID provide training support to tens of thousands of health workers in malaria case management, diagnostic testing, and prevention of malaria during pregnancy. Last year, PMI trained 38,000 health workers in IPTp delivery and procured 7 million preventive treatments for pregnant women.
We know integration is central to our success.
Integrated approaches that promote comprehensive prevention and control for pregnant women and children — as well as efforts to strengthen the health system — need to be implemented and taken to scale at country level. At the community level, MCSP is training CHWs to recognize signs of malaria and refer suspected cases to facilities. We’re also strengthening health facilities in pre-elimination efforts and training providers on how to actively detect and treat malaria cases using rapid diagnostic tests. And nationally, MCSP supports government health ministries to combat malaria in pregnancy through lifesaving and cost-effective tools.
Journey with us to Rwanda and Nepal, where you can see these efforts bearing fruit on the ground.

A dream realized: Rwandan community health worker champions child health
Monique Nirere had a lifelong passion for health care, but only recently, at age 40, was able to help improve the health of her rural village by becoming a community health worker.
READ MOREEntering the Crucial “Elimination Phase,” Nepal Steps Forward to End Malaria
In the fight against malaria, Nepal has accomplished what many other countries in the developing world can only aspire to — reducing by more than half the number of confirmed cases of the often fatal disease in just 6 years.
READ MORE